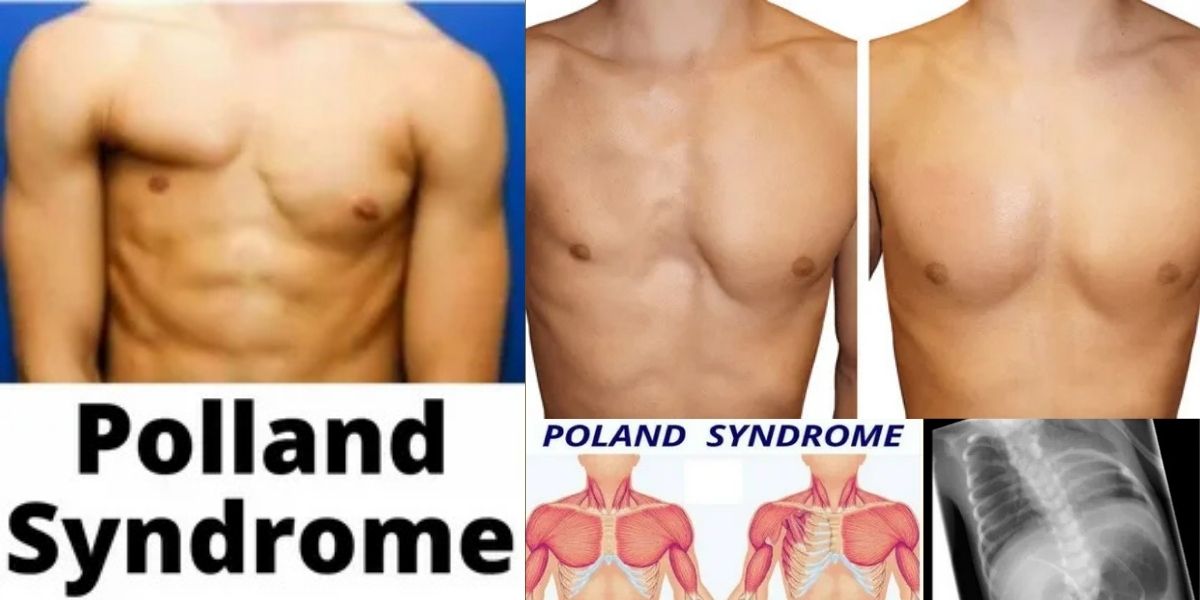
Poland Syndrome: Poland syndrome is a rare congenital condition that primarily manifests as the underdevelopment or total absence of the chest muscles on one side of the body. While often identified at birth due to visible physical asymmetries, many individuals do not receive a formal diagnosis until they reach puberty, when the body’s natural growth emphasizes the lack of muscle development in the thoracic region. This condition typically involves the pectoralis major muscle, but its reach can extend to the ribs, the breast tissue, and even the hand on the same side, creating a complex clinical picture that requires a highly individualized approach to care. Because the severity ranges from mild aesthetic differences to functional limitations in the upper extremities, understanding the full spectrum of the disorder is essential for patients and families seeking the best long-term outcomes.
Navigating the journey of a rare disease often involves a steep learning curve for both patients and healthcare providers who may not encounter the condition frequently. Recent advancements in medical technology, particularly in the fields of 3D imaging and reconstructive surgery, have significantly expanded the options available for managing the physical markers of the syndrome. This article aims to provide a deep, authoritative dive into the mechanical, biological, and psychological aspects of the condition, offering a roadmap for those seeking to understand how modern medicine addresses these unique developmental challenges. By positioning this information within a broader context of pediatric development and surgical innovation, we can better appreciate the resilience of individuals living with this condition and the specialized care that supports their well-being.
Defining the Core Characteristics of Poland Syndrome
At its most fundamental level, Poland syndrome is characterized by the unilateral agenesis or hypoplasia of the pectoralis major muscle, specifically the sternocostal head which attaches to the breastbone and ribs. This absence creates a hollowed or concave appearance on one side of the chest, often accompanied by a higher-than-normal nipple placement or the absence of an areola. In many clinical cases, the pectoralis minor, a smaller muscle located beneath the major, is also missing, which can further impact the stability of the shoulder girdle. The condition is noticeably more prevalent in males than in females and shows a strong statistical preference for affecting the right side of the body, though the reasons for this laterality remain a subject of ongoing medical inquiry.
Beyond the muscular deficits, the syndrome often presents with a variety of associated skeletal and soft tissue anomalies that define its complexity. Some individuals may experience hypoplasia of the subcutaneous fat, making the skin appear thinner and the underlying ribs more prominent, while others may have structural rib defects that lead to a slight rotation of the sternum. In female patients, the underdevelopment of breast tissue on the affected side is a primary concern, often requiring a combination of thoracic and plastic surgery to achieve symmetry. Because the condition is sporadic and rarely inherited, it presents as a unique developmental event during gestation, leading to a wide range of phenotypic expressions that make every patient’s experience distinct.
The Vascular Theory of Subclavian Artery Disruption
The most widely accepted explanation for the development of this condition is the Subclavian Artery Supply Disruption Sequence, which suggests that a temporary blockage or reduction in blood flow occurs during the sixth week of embryonic development. During this critical window, the blood vessels that eventually become the subclavian and vertebral arteries are responsible for delivering nutrients to the tissues that form the chest wall and the upper limbs. If the blood supply is compromised—whether due to a physical obstruction, a rapid growth spurt of the surrounding tissues, or a localized vascular event—the structures that were supposed to develop from those specific embryonic buds may fail to form correctly. This theory explains why the muscle loss and hand abnormalities often occur on the same side, as they share a common vascular origin.
While the specific trigger for this vascular disruption remains unknown, researchers have explored various factors including environmental influences and rare genetic predispositions. Most cases appear to be sporadic, occurring in families with no prior history of the disorder, which supports the idea of a localized event in the womb rather than a heritable trait. However, some studies have identified rare familial clusters that suggest an autosomal dominant inheritance pattern in specific populations, though no single gene has been definitively linked to the condition across the board. Understanding this vascular foundation is crucial for clinicians, as it helps them assess for other potential anomalies in the heart, lungs, or kidneys that might have been affected by the same developmental timeframe.
Understanding Symbrachydactyly and Hand Involvement
One of the most striking associations in many cases of this disorder is the presence of hand abnormalities, collectively referred to as symbrachydactyly. This condition involves the presence of abnormally short fingers (brachydactyly) that are often joined together by skin or tissue webbing (syndactyly). In more severe presentations, some of the middle bones of the fingers may be entirely missing, or the hand may appear significantly smaller than the one on the unaffected side. The link between the chest and the hand is rooted in the same embryonic developmental window, where the disruption of the brachial artery affects the distal growth of the limb buds. Not every patient with the thoracic symptoms will have hand involvement, but when present, it often requires early intervention from hand specialists to maximize functional utility.
The impact of symbrachydactyly goes beyond the aesthetic, as it can influence fine motor skills and the ability to perform complex tasks during childhood. Physical and occupational therapy are often introduced early to help the child adapt and develop strength in the affected hand, while surgical procedures such as syndactyly release are commonly performed in the toddler years. These surgeries aim to separate fused fingers and, in some cases, lengthen existing digits to improve the grip and pinch functions. For many families, the hand involvement is the first visible sign of the syndrome, prompting a more thorough evaluation of the chest and shoulder to identify the full extent of the condition before the child enters the social environment of school.
Variations in Physical Presentation and Severity
The phenotypic spectrum of Poland syndrome is incredibly broad, meaning that no two individuals will have an identical presentation. In mild cases, the only sign might be a slightly smaller pectoralis muscle that is only noticeable when the individual performs specific movements, like pushing or lifting. These individuals may live most of their lives without knowing they have a named medical condition, only discovering it later during a routine physical or when they begin a bodybuilding or fitness regimen that reveals the asymmetry. In these instances, the functional impact is virtually non-existent, and the condition is viewed primarily through a lens of cosmetic preference or minor structural variation.
Conversely, severe cases can involve significant skeletal changes, such as the complete absence of several ribs or the presence of a “flail chest,” where the lack of structural support on one side affects breathing mechanics. In these situations, the thoracic cage may appear deeply concave, and the internal organs like the heart or lungs may be more vulnerable to external pressure due to the lack of protective muscle and bone. Some patients also exhibit dextrocardia, where the heart is located on the right side of the chest instead of the left, further complicating the clinical management. This vast range of severity necessitates a multidisciplinary team of experts—including thoracic surgeons, cardiologists, and plastic surgeons—to ensure that all aspects of the patient’s health are monitored and addressed according to their specific needs.
Diagnosis Protocols in Early Childhood and Puberty
Diagnosing the condition is primarily a clinical process, relying on a thorough physical examination and a review of the patient’s developmental history. In newborns, the presence of hand webbing or a noticeable depression in the chest is usually enough to trigger an investigation. However, for many children, the muscular deficit is masked by subcutaneous fat during infancy and early childhood. It is often not until the onset of puberty, when the male chest begins to broaden or the female breasts begin to develop, that the asymmetry becomes glaringly apparent. This “delayed” discovery can be distressing for adolescents, making it vital for pediatricians to be aware of the subtle signs of muscle hypoplasia during routine checkups.
To confirm the diagnosis and assess the extent of the involvement, physicians may utilize imaging technologies such as Computed Tomography (CT) or Magnetic Resonance Imaging (MRI). These scans allow doctors to visualize exactly which muscles are missing and whether the underlying rib cage or lung tissue is affected. In some cases, an X-ray of the hands and chest is sufficient to identify skeletal anomalies or the characteristic absence of the sternocostal head. Once the structural layout is understood, a long-term care plan can be established, which might involve conservative monitoring during growth or planning for reconstructive surgeries once the patient reaches skeletal maturity.
Psychological Resilience and Body Image Challenges
The psychological impact of living with a visible physical difference cannot be overstated, particularly during the vulnerable years of adolescence and young adulthood. Individuals with Poland syndrome often report feelings of self-consciousness when participating in activities that require them to reveal their chest, such as swimming or changing in a locker room. This can lead to social withdrawal, a lack of self-confidence, and a persistent focus on the perceived “flaw” in their appearance. While many patients develop incredible resilience and adapt well to their condition, others may struggle with body dysmorphia or anxiety related to how they are perceived by their peers.
Support groups and psychological counseling play a critical role in the holistic management of the syndrome. By connecting with others who share similar experiences, patients can find a sense of community and validation that helps mitigate the isolation of having a rare disease. Mental health professionals can provide tools for coping with social anxiety and building a positive self-image that is not solely defined by physical symmetry. It is important for parents and clinicians to recognize that the emotional well-being of the patient is just as important as their physical reconstruction, as a healthy mindset is the foundation for a successful long-term outcome and high quality of life.
Surgical Innovations: The Shift to 3D Custom Implants
In the past, reconstructive options for the chest were often limited to large, invasive procedures like the latissimus dorsi muscle flap, which involved moving muscle from the back to the front. While effective, these surgeries left significant scarring and required a long recovery period. Today, the landscape of treatment for Poland syndrome has been revolutionized by the development of custom-designed 3D silicone implants. Using high-resolution CT scans, engineers can create a digital model of the patient’s chest wall and design an implant that perfectly fits the unique contours of their skeletal structure. This allows for a much more precise restoration of symmetry with significantly less trauma to the surrounding tissues.
These custom implants are made of solid, medical-grade silicone, which feels similar to muscle tissue and does not carry the risk of rupture or leakage associated with gel-filled implants. The surgery is typically performed through a small incision in the armpit or under the breast fold, minimizing visible scarring and allowing for a faster return to daily activities. Because the implant is designed specifically for the individual, it can fill the hollowed area of the chest with a level of accuracy that was previously impossible to achieve. This approach has become the gold standard for many male patients and is frequently used as a foundation for more complex reconstructions in female patients, offering a durable and aesthetically pleasing solution.
Breast Reconstruction Strategies for Female Patients
For female patients, the underdevelopment of the breast tissue adds an extra layer of complexity to the reconstructive process. The goal is not only to restore the volume of the breast but also to ensure that the nipple-areola complex is positioned symmetrically and that the overall contour of the chest wall is addressed. Often, this requires a staged approach, beginning with a tissue expander to gradually stretch the skin on the affected side. Once enough skin has been created, the expander is replaced with a permanent breast implant, sometimes in conjunction with a custom chest wall implant to fill the underlying muscular deficit.
In some cases, surgeons may recommend a “hybrid” approach that combines implants with autologous tissue transfer. This might involve using a small portion of the patient’s own muscle or fat to create a more natural look and feel. For example, a latissimus dorsi flap can provide both volume and a natural “cushion” over an implant, which is particularly useful if the skin on the chest is very thin. Modern techniques also focus on the unaffected breast, sometimes performing a lift or augmentation to ensure that both sides match as closely as possible in shape, size, and projection. The result is a comprehensive reconstruction that addresses both the skeletal and soft tissue aspects of the condition, significantly improving the patient’s body image.
The Role of Fat Grafting and Lipofilling in Contouring
Fat grafting, also known as lipofilling, has emerged as a powerful adjunctive tool in the treatment of Poland syndrome. This procedure involves harvesting fat from one area of the patient’s body—such as the abdomen or thighs—via liposuction, processing it, and then injecting it into the chest area to refine the contours. It is particularly effective for smoothing out the edges of an implant, filling in small hollows near the collarbone, or adding a layer of natural softness to the reconstructed breast. Because the patient’s own tissue is used, there is no risk of rejection, and the results can be quite natural-looking.
While fat grafting may not be sufficient on its own to correct severe muscle deficits, it is an excellent way to achieve the “fine-tuning” required for a truly symmetric result. Some patients may require multiple rounds of lipofilling, as a percentage of the transferred fat is naturally reabsorbed by the body over time. However, once the remaining fat cells establish a blood supply, the results are permanent. This technique allows surgeons to address the subtle transitions between the chest and the shoulder or the breast and the armpit, which are often the areas where the muscular absence is most apparent. It represents a shift toward more refined, less invasive methods of achieving aesthetic harmony.
Functional Limitations and Physical Therapy Adaptation
While much of the focus on this syndrome is aesthetic, there are functional considerations that need to be addressed, particularly regarding shoulder and arm strength. The pectoralis major is a key muscle for movements such as internal rotation, adduction (bringing the arm toward the body), and pushing. Individuals missing this muscle may find certain tasks more fatiguing or may lack the explosive power needed for specific sports. However, the human body is remarkably adaptable, and many patients naturally compensate by strengthening other muscles in the shoulder girdle, such as the deltoids, the serratus anterior, and the latissimus dorsi.
Physical therapy can be an invaluable asset in this adaptation process. A therapist can design a targeted exercise program that focuses on maximizing the strength and range of motion in the compensatory muscles, ensuring that the shoulder joint remains stable and functional. Many individuals with the syndrome lead very active lives, participating in competitive sports, weightlifting, and manual labor without significant impairment. By focusing on functional movement patterns rather than just the missing anatomy, patients can overcome most physical limitations. It is also important for coaches and trainers to be aware of the condition so they can modify exercises to prevent overuse injuries in the compensatory muscle groups.
Associated Conditions: From Moebius to Klippel-Feil
Poland syndrome does not always occur in isolation; it is occasionally associated with other rare congenital disorders that share a similar developmental timeline. One of the most notable is Moebius syndrome, a rare neurological condition characterized by the paralysis of the facial nerves, which prevents individuals from smiling, frowning, or moving their eyes laterally. The combination of these two conditions is sometimes referred to as Poland-Moebius syndrome, and it is thought to result from a more extensive vascular disruption that affects both the subclavian artery and the blood supply to the brainstem.
Other associated conditions include Klippel-Feil syndrome, which involves the abnormal fusion of the cervical vertebrae, and Sprengel deformity, where the shoulder blade is located too high on the back. These associations highlight the importance of a comprehensive systemic evaluation when the syndrome is first identified. Patients may also present with renal agenesis (a missing kidney) or vertebral abnormalities. While these complications are rare, they underscore the need for a multidisciplinary approach to care that looks beyond the chest wall. By identifying these issues early, healthcare providers can ensure that the patient receives the appropriate monitoring and interventions to prevent long-term health complications.
Comparison of Common Treatment Modalities
| Treatment Option | Primary Goal | Best Suited For | Key Advantage |
| Custom 3D Implant | Restore chest wall symmetry | Male & Female patients | Anatomically perfect fit |
| Latissimus Dorsi Flap | Replace missing muscle bulk | Severe cases / Breast recon | Uses patient’s own tissue |
| Fat Grafting | Fine-tuning and contouring | Mild cases / Post-implant | Minimally invasive; natural feel |
| Tissue Expansion | Create skin for breast implant | Female patients | Prepares for permanent recon |
| Physical Therapy | Optimize shoulder function | All patients | Improves strength & mobility |
Long-Term Outlook and Quality of Life Outcomes
The long-term outlook for individuals with Poland syndrome is generally excellent. Most patients go on to lead full, healthy lives with no significant impact on their life expectancy or general health. Studies on long-term outcomes show that once the initial reconstructive phase is complete, patient satisfaction with their appearance and functional abilities is very high. While the journey through multiple surgeries can be challenging, the resulting improvement in self-esteem and the reduction in social anxiety are often life-changing. Most individuals find that they can return to all their favorite activities, from sports to professional careers, with few restrictions.
As the medical community continues to refine its techniques, the quality of results continues to improve. Innovations in regenerative medicine, such as the use of stem cells to improve fat graft survival or the development of even more bio-compatible materials for implants, hold promise for the future. The focus is shifting toward not just “fixing” a deformity, but providing a reconstruction that is so natural it becomes a non-issue in the patient’s daily life. With the right combination of surgical expertise, psychological support, and functional training, the hurdles associated with this rare condition can be successfully navigated, allowing the individual’s true potential to shine through.
“The primary objective in managing this condition is not just the restoration of symmetry, but the restoration of the patient’s confidence in their own body.” — Dr. Julian Marra, Reconstructive Surgeon.
Navigating the Healthcare System and Specialist Care
Finding the right medical team is perhaps the most important step for anyone dealing with a rare diagnosis. Because Poland syndrome involves multiple systems—muscular, skeletal, and sometimes vascular—it is essential to seek out specialists who have specific experience with this disorder. Often, this means traveling to a major academic medical center or a specialized pediatric hospital where multidisciplinary clinics are available. A team approach ensures that the hand surgeon, the plastic surgeon, and the physical therapist are all on the same page, coordinating their efforts to minimize the number of surgeries and optimize the timing of each intervention.

Patients and their families should feel empowered to ask questions and seek second opinions. It is important to understand the pros and cons of different surgical techniques, such as the choice between a custom implant and a muscle flap. Being an informed advocate for one’s own health—or the health of a child—can lead to better decision-making and a more satisfying surgical outcome. Additionally, many insurance companies may initially view these procedures as “cosmetic,” so working with a team that knows how to document the medical necessity of reconstruction for congenital anomalies is vital for securing coverage.
Myths and Misconceptions Surrounding the Condition
One of the most common myths about Poland syndrome is that it is the result of something the mother did during pregnancy, such as diet, exercise, or stress. It is crucial to clarify that this is a sporadic vascular event that occurs very early in gestation, and there is no evidence to suggest that maternal behavior plays any role in its development. Clearing this misconception is vital for reducing the guilt that many parents feel when their child is born with a congenital difference. Understanding that it is a random developmental “hiccup” can help families focus on the path forward rather than searching for a cause that doesn’t exist.
Another misconception is that the condition will “go away” or that the muscle will eventually grow in with exercise. While exercise can strengthen the surrounding muscles and improve the overall appearance of the chest, it cannot create muscle tissue where the embryonic precursors never existed. Attempting to “train away” the asymmetry through heavy weightlifting can sometimes make the difference more noticeable, as the unaffected side grows while the affected side remains flat. Education on what can and cannot be achieved through fitness alone helps patients set realistic goals and decide if and when surgical intervention is the right choice for them.
Conclusion
Poland syndrome is a complex but manageable condition that touches the lives of individuals in diverse ways, from minor aesthetic variances to significant structural challenges. By understanding the underlying vascular causes and the wide array of modern reconstructive options, patients and their families can approach the future with a sense of hope and clarity. The evolution of 3D printing and fat grafting has provided more natural and less invasive solutions than ever before, ensuring that the physical markers of the condition no longer have to define a person’s identity or limit their potential. Ultimately, with a multidisciplinary approach that prioritizes both physical symmetry and psychological well-being, individuals can thrive and lead lives defined by resilience rather than by the absence of a muscle.
FAQs
Is Poland syndrome a genetic condition that I can pass on to my children?
In the vast majority of cases, this condition is sporadic, meaning it occurs randomly during fetal development with no family history. While there are extremely rare instances where the condition has appeared in multiple generations, for most people, the risk of passing Poland syndrome on to their children is considered very low.
At what age is it best to have surgery for the chest deformity?
For most patients, it is recommended to wait until skeletal maturity is reached, usually in the late teens or early twenties, to ensure the chest wall and breast tissue have finished developing. However, hand surgeries to address symbrachydactyly associated with Poland syndrome are typically performed much earlier, often between the ages of one and four, to help with the child’s motor development.
Will insurance cover the cost of a custom 3D implant?
Many insurance providers will cover reconstructive surgery for congenital anomalies like Poland syndrome, as it is considered a corrective procedure rather than a purely cosmetic one. It is important to work with your surgical team to provide the necessary medical documentation, including imaging and clinical evaluations, to demonstrate that the procedure is necessary for restoring normal anatomy.
Can I still play sports or lift weights if I have this condition?
Yes, most people with the condition are fully capable of participating in sports and weightlifting, though they may notice some lack of strength in specific pushing or pulling movements. Physical therapy can help you develop compensatory strength in other muscle groups, and many athletes with Poland syndrome have successfully competed at very high levels by focusing on overall functional fitness.
What is the recovery time after a custom chest implant surgery?
The recovery for a custom silicone implant procedure is relatively quick compared to traditional muscle flap surgeries, with most patients returning to light daily activities within one to two weeks. Full physical activity and heavy lifting are typically restricted for about six to eight weeks to ensure the implant has settled and the internal tissues have healed properly, but long-term maintenance for these solid implants is minimal.