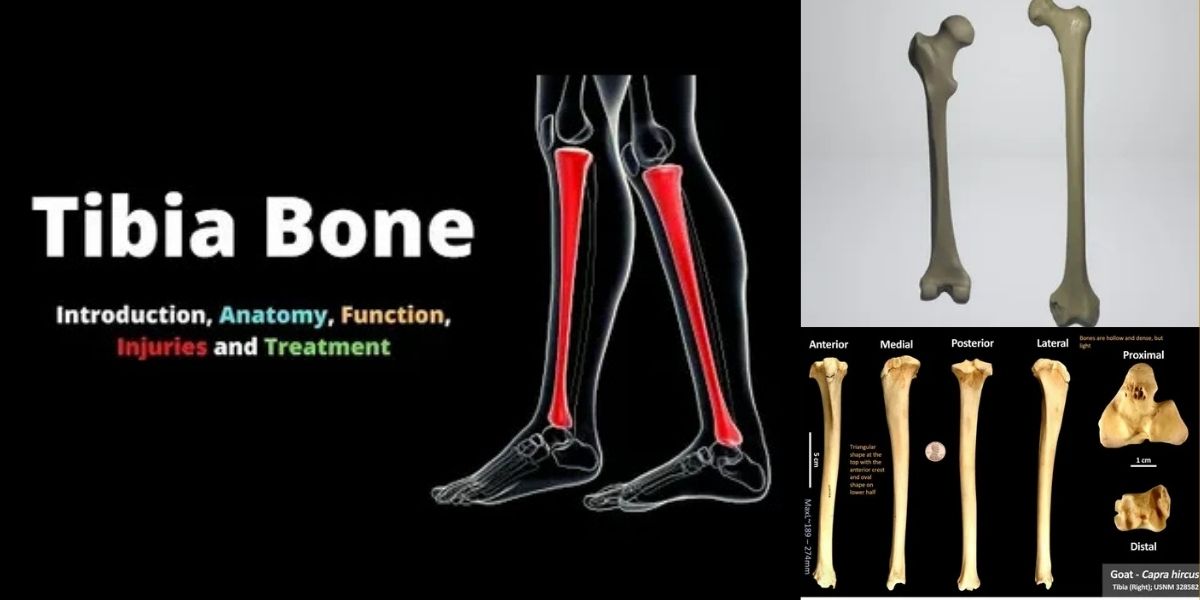
Tibia Bone: The human leg is an engineering marvel designed to withstand immense force, and at the center of this structural masterpiece sits the tibia bone. Often referred to as the shinbone, this osseous structure is the larger, stronger, and anterior (front) of the two bones in the leg below the knee. It connects the knee to the ankle and is responsible for bearing the vast majority of your body weight during daily activities like walking, jumping, and running. Because of its location and load-bearing responsibility, the tibia is one of the most commonly fractured long bones in the body, making it a frequent subject of orthopedic study and care.
Understanding the complexity of the tibia requires looking beyond just its hard exterior to see how it integrates with muscles, nerves, and blood vessels to facilitate movement. Whether you are an athlete dealing with shin splints, a patient recovering from trauma, or simply interested in human anatomy, grasping the role of this vital bone provides a window into how our bodies maintain stability against gravity. This comprehensive guide explores every facet of the shinbone, from its microscopic architecture to its critical role in biomechanics and the latest advancements in treating tibial injuries.
Architectural Overview of the Tibia
The tibia is classified as a long bone, characterized by a hard, dense shaft and two articular ends that form joints. The proximal end, which is the top part closest to the thigh, flares out to form the tibial plateau. This flat surface is crucial because it acts as the foundation for the femur (thigh bone) to rest upon, creating the knee joint. The surface is covered in articular cartilage and houses the menisci, which act as shock absorbers. Without this widened platform, the high pressure of body weight would not be distributed evenly, leading to rapid joint degeneration.
Moving down from the knee, the bone tapers into a triangular shaft. This shape is not accidental; the triangular cross-section provides exceptional resistance to bending and twisting forces. The anterior crest, which is the sharp ridge you can feel running down the front of your shin, is located here. Because the tibia is subcutaneous—meaning it sits just below the skin without a significant cushion of muscle—it is incredibly vulnerable to direct impact. This lack of protection is why bumping your shin is so disproportionately painful compared to other areas of the body.
The Relationship Between Tibia and Fibula
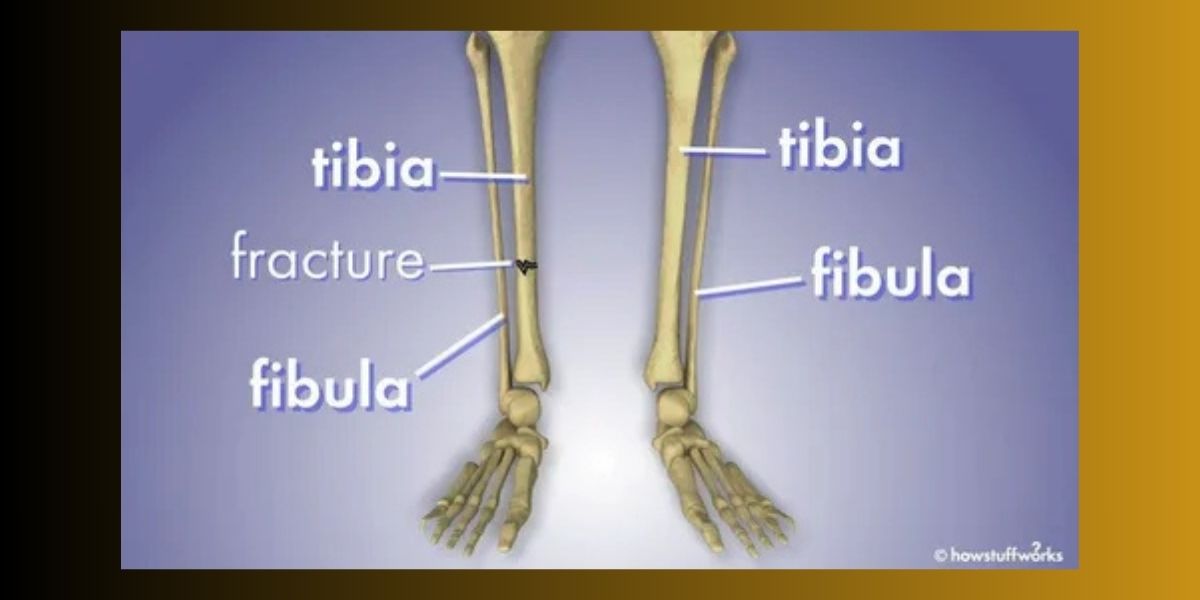
While the tibia bone takes the spotlight for weight-bearing, it does not work alone; it is paired with the fibula, a thinner bone running parallel to it on the lateral (outer) side of the leg. These two bones are connected by a strong sheet of connective tissue called the interosseous membrane. This membrane does more than just hold the bones together; it transfers forces between them and serves as a vital attachment point for deep muscles. The relationship is symbiotic, yet unequal in terms of load.
The tibia bears approximately 85% to 90% of the body’s weight, leaving the fibula to handle the remainder while focusing primarily on muscle attachment and ankle stability. At the ankle joint, the tibia forms the medial malleolus (the inner ankle bump), while the fibula forms the lateral malleolus (the outer ankle bump). Together, they create a mortise, a bracket-like shape that locks the talus bone of the foot in place. This partnership ensures that while the tibia handles the heavy lifting, the fibula provides the lateral stability needed for varied terrain.
Proximal Tibial Anatomy and Knee Function
The top of the tibia is a complex landscape known as the tibial plateau, consisting of the medial and lateral condyles. These condyles are concave to accept the convex femoral condyles, functioning much like a ball-and-socket mechanism, though flatter. Between these two condyles lies the intercondylar eminence, a bony spine where the Anterior Cruciate Ligament (ACL) and Posterior Cruciate Ligament (PCL) attach. These ligaments are the primary stabilizers of the knee, preventing the tibia from sliding too far forward or backward relative to the femur.
Damage to the proximal tibia can have devastating effects on knee mechanics. A fracture here, often called a plateau fracture, disrupts the smooth cartilage surface. If this surface heals unevenly, it creates a rough interface that grinds against the femur with every step, rapidly accelerating the onset of osteoarthritis. Orthopedic surgeons prioritize restoring this articular surface to near-perfect smoothness during surgery to preserve the patient’s long-term mobility and delay the need for knee replacement.
The Tibial Shaft and Stress Distribution
The diaphysis, or shaft, of the tibia is optimized for vertical compression. As you walk, ground reaction forces travel up through the foot and into the tibial shaft. The bone is thickest in the upper and middle thirds and thins out as it approaches the ankle. Interestingly, the transition zone between the middle and lower third is the weakest point structurally and has the poorest blood supply. This specific anatomical quirk makes the lower third of the tibia the most common site for fractures and delayed healing.
The shaft is also dynamic, constantly remodeling itself in response to stress via a process known as Wolff’s Law. Athletes who engage in high-impact sports like gymnastics or distance running often develop denser, thicker tibial shafts over time. Conversely, a sedentary lifestyle leads to a reduction in bone density. This responsiveness highlights the tibia bone as a living tissue that adapts to the demands placed upon it, reinforcing itself where mechanical stress is highest.
Distal Tibia and Ankle Mechanics
At its lower end, the tibia widens again to form the ceiling of the ankle joint, known as the plafond. The medial malleolus extends downward from the medial side, providing a bony buttress that prevents the foot from rolling inward excessively. This distal region is covered with hyaline cartilage, allowing for smooth articulation with the talus bone. The intricate geometry of the distal tibia is essential for the hinge-like motion of the ankle, allowing for dorsiflexion (lifting the foot) and plantarflexion (pointing the toe).
Injuries to the distal tibia, such as pilon fractures, are notoriously difficult to treat because the bone is driven into the ankle joint, often shattering the cartilage. The soft tissue envelope here is thin, and swelling can be severe, complicating surgical intervention. Successful management of the distal tibia focuses on restoring the alignment of the ankle mortise. Even a millimeter of displacement in this area can significantly alter contact pressures in the ankle, leading to chronic pain and instability.
Muscular Attachments and Movement
The tibia serves as an anchor for many of the lower body’s most powerful muscles. On the anterior aspect, the tibialis anterior muscle runs alongside the lateral face of the shaft. This muscle is responsible for dorsiflexion, which is the action of pulling your toes up toward your shin. Without a functioning tibialis anterior, a person would suffer from “foot drop,” requiring them to lift their leg unnaturally high to avoid dragging their toes while walking.
On the posterior (back) side, the tibia provides attachment for the soleus and other deep flexor muscles. The expansive surface area of the posterior tibia allows these muscles to generate the massive force required for propulsion during running and jumping. Additionally, the patellar tendon attaches to the tibial tuberosity, a bump on the front of the upper tibia. This attachment point allows the quadriceps muscles to extend the knee, a fundamental movement for standing up, kicking, and climbing stairs.
Blood Supply and Vascular Considerations
Bone viability depends entirely on blood flow, and the tibia presents a unique challenge in this regard. The nutrient artery enters the bone through a small hole in the posterior upper third of the shaft. Once inside, it branches out to supply the marrow and the inner cortex of the bone. However, the outer surface of the bone relies on the periosteum—a thin, vascularized membrane wrapping the bone—for its blood supply.
In the lower third of the tibia, this periosteal blood supply is sparse, and the nutrient artery’s reach is limited. This creates a “watershed area” of low vascularity. When a high-energy fracture occurs, the periosteum is often stripped away, and the nutrient artery may be severed. This leaves the bone segments isolated from their blood source, significantly increasing the risk of non-union (failure to heal) or malunion. Surgeons must be incredibly careful to preserve whatever soft tissue attachments remain during reconstruction to maintain blood flow.
Common Tibial Fractures and Trauma
Tibial fractures are the most common long bone fracture, largely due to the bone’s exposed position and weight-bearing role. These breaks range from simple, non-displaced hairline fractures to complex, open fractures where the bone penetrates the skin. Open fractures are a medical emergency carrying a high risk of infection, as bacteria can easily enter the sterile environment of the bone marrow. The nature of the break often dictates the treatment, with high-energy impacts (like car accidents) causing comminuted fractures where the bone shatters into multiple pieces.
Treatment for a broken tibia bone has evolved significantly. While casting is still used for stable, aligned fractures, modern orthopedics favors intramedullary nailing for shaft fractures. This involves inserting a metal rod down the hollow center of the bone, locked in place with screws at both ends. This internal splint allows patients to bear weight much sooner than casting, which promotes faster healing through micromotion and reduces the complications associated with prolonged immobility.
Shin Splints and Stress Injuries
Not all tibial issues are acute fractures; chronic overuse injuries are rampant, particularly Medial Tibial Stress Syndrome (MTSS), commonly known as shin splints. This condition involves inflammation of the periosteum where muscles attach to the tibia. It is typically caused by repetitive impact on hard surfaces or a sudden increase in training volume. The pain is usually felt along the inner edge of the shinbone and can be debilitating if not managed with rest and biomechanical correction.
If ignored, shin splints can progress into a tibial stress fracture. Unlike a traumatic break, a stress fracture is a microscopic crack that forms when the bone’s remodeling process cannot keep up with the damage caused by repetitive loading. These injuries are insidious, often presenting as a dull ache that worsens with activity and subsides with rest. Diagnosis often requires an MRI or bone scan, as stress fractures may not appear on standard X-rays until the bone begins to heal and form a callus.
Pediatric Considerations and Growth Plates
In children and adolescents, the tibia behaves differently due to the presence of physis, or growth plates, located at both the proximal and distal ends. These cartilaginous zones are where longitudinal bone growth occurs. Because the growth plate is softer than the surrounding calcified bone, it is often the weak link in the chain during trauma. A force that might sprain a ligament in an adult can cause a growth plate fracture in a child, potentially threatening future growth if the plate closes prematurely.
Osgood-Schlatter disease is another condition specific to the developing tibia. It manifests as a painful lump below the knee at the tibial tuberosity. This occurs during growth spurts when the bone grows faster than the muscles and tendons, causing the patellar tendon to pull tightly against its attachment point. While painful, it is a self-limiting condition that typically resolves once the skeletal system reaches maturity, leaving behind a prominent but harmless bony bump.
Surgical Interventions and Technology
Advancements in medical technology have revolutionized how surgeons approach tibial reconstruction. Computer-assisted navigation and 3D printing now allow for precise planning of complex deformity corrections and fracture reductions. For patients with severe bone loss due to trauma or tumor resection, distraction osteogenesis (Ilizarov technique) can be used. This involves an external fixator frame that slowly pulls the bone segments apart, stimulating new bone to grow in the gap, effectively lengthening the tibia.

Biological augmentation is another frontier in treating the tibia bone. The use of bone morphogenetic proteins (BMPs) and stem cell grafting helps stimulate healing in stubborn non-unions. These biological adjuncts signal the body to accelerate the repair process, bridging gaps that natural healing might fail to close. As these technologies become more accessible, the prognosis for catastrophic tibial injuries continues to improve, reducing amputation rates and restoring function to higher levels than previously possible.
Rehabilitation and Physical Therapy
Healing the bone is only half the battle; rehabilitating the surrounding soft tissue is crucial for a full recovery. After a period of immobilization, the muscles surrounding the tibia—specifically the calf and quadriceps—will atrophy significantly. Physical therapy focuses initially on range of motion, particularly at the ankle and knee, to prevent stiffness. Stiffness in the ankle joint following a tibial fracture is a common complication that can permanently alter a patient’s gait.
As the bone consolidates, therapy shifts toward load-bearing exercises and proprioception training. Proprioception is the body’s ability to sense its position in space, a sense that is often damaged alongside the bone and nerves. Balance exercises, such as standing on a wobble board, help retrain the nervous system to stabilize the leg. Without this neuromuscular re-education, the patient remains at a higher risk for re-injury due to a lack of stability and coordination.
Nutritional Support for Bone Health
The structural integrity of the tibia is heavily influenced by systemic health and nutrition. Calcium and Vitamin D are the cornerstones of bone density, but other micronutrients like magnesium, Vitamin K2, and protein play vital roles. A deficiency in these nutrients renders the tibia more susceptible to stress fractures and osteoporosis later in life. For athletes and the elderly, monitoring nutritional intake is a proactive strategy to maintain the resilience of weight-bearing bones.

Systemic conditions like diabetes and smoking also have a profound negative impact on the tibia. Nicotine constricts blood vessels, reducing the already precarious blood supply to the lower leg, while high blood sugar impairs the immune response and healing rate. Orthopedic surgeons often require patients to stop smoking before performing elective tibial surgeries, such as osteotomies, because the risk of the bone failing to knit together is drastically higher in smokers.
The Evolutionary Perspective
The human tibia is unique among primates, adapted specifically for habitual bipedalism. In our ape ancestors, the tibia is adapted for climbing, with different articular angles and density distributions. The human tibia is straighter and vertically aligned directly under the femur to support prolonged upright walking. This evolution allows for energy-efficient striding but places vertical compression loads on the bone that quadrupeds do not experience.
This evolutionary adaptation comes with trade-offs. The vertical orientation makes the tibia excellent at handling compression but vulnerable to torsional (twisting) and shearing forces, such as those experienced in skiing accidents or football tackles. Understanding this evolutionary context helps explains why certain injuries are so prevalent in humans; we are using a structure adapted for efficient walking to perform high-velocity, multi-directional sports that push the bone’s biological limits.
Comparison: Tibia vs. Fibula
To better understand the distinct roles of the lower leg bones, it is helpful to view them side-by-side. The following table highlights the key functional and anatomical differences between these two partners.
| Feature | Tibia | Fibula |
| Primary Function | Weight-bearing (approx. 85-90%) | Muscle attachment & ankle stability |
| Location | Medial (inner side of leg) | Lateral (outer side of leg) |
| Thickness | Thick, triangular shaft | Thin, irregular shaft |
| Knee Connection | Articulates directly with femur | Does not touch the femur |
| Ankle Feature | Forms Medial Malleolus | Forms Lateral Malleolus |
| Palpability | Easily felt (shinbone) | Mostly buried under muscle |
| Fracture Healing | Slower due to precarious blood supply | Generally faster healing |
Conclusion
The tibia bone is far more than a simple strut of calcium; it is a dynamic, load-bearing pillar that is central to human locomotion. From the complex geometry of the knee plateau to the stable mortise of the ankle, the tibia’s anatomy is a testament to the requirements of bipedal movement. Its exposure makes it vulnerable, yet its ability to remodel and heal demonstrates the resilience of the human skeletal system.
Maintaining tibial health requires a multifaceted approach involving proper nutrition, smart training loads, and immediate attention to pain. Whether you are navigating recovery from a fracture or looking to prevent future injuries, respecting the limits and needs of your shinbone is essential. As medical science advances, our ability to repair and reinforce this critical bone ensures that even after severe trauma, patients can return to standing tall and moving freely.
FAQs
What is the recovery time for a broken tibia bone?
Recovery timelines vary significantly based on the severity of the break. A simple stress fracture may heal in 6 to 8 weeks with rest, while a severe shaft fracture treated with surgery typically takes 4 to 6 months for full bony union. However, complete return to high-impact sports or rigorous labor can take up to a year, as the soft tissue and muscle strength require extensive rehabilitation even after the bone has technically healed.
Can you walk with a fractured tibia?
Generally, you cannot and should not walk on an acute tibial fracture. Because the tibia bears 90% of your body weight, attempting to walk on a break can displace the bone segments, causing severe pain and further damage to nerves and blood vessels. In cases of minor stress fractures, walking might be possible but painful; however, most tibial injuries require crutches or a walking boot to offload weight and allow the healing process to begin.
Why do shin splints hurt the tibia so much?
Shin splints, or Medial Tibial Stress Syndrome, cause pain because the connective tissue (periosteum) covering the tibia becomes inflamed. This tissue is rich in nerve endings, making it highly sensitive. The pain is caused by the muscles pulling repeatedly on this inflamed wrapping of the bone, creating a sharp, burning sensation along the inner edge of the shin that intensifies during activity.
Is the tibia the strongest bone in the body?
While the tibia is incredibly strong and able to support significant weight, it is not the strongest bone in the body; that title belongs to the femur (thigh bone). The femur is larger, denser, and protected by massive muscle groups. However, the tibia is the strongest weight-bearing bone below the knee and has a high density to handle the direct impact forces transferred from the foot.
What is the “bump” on the top of the tibia below the knee?
The bump located just below the kneecap on the front of the tibia is called the tibial tuberosity. It serves as the attachment point for the patellar tendon, which connects the kneecap and quadriceps muscles to the lower leg. In adolescents, this area can become swollen and painful due to Osgood-Schlatter disease, but in adults, it is a normal anatomical landmark used by surgeons and therapists to orient the leg.